Today, obesity is recognized by national medical organizations as a chronic disease, not merely a lifestyle issue.1,2 The American Medical Association considers obesity to be a disease state that requires a range of interventions.1 This will help you understand the struggles individuals with obesity face with losing weight and maintaining weight loss.
| For many people who have obesity, willpower and lifestyle modifications alone are not enough to maintain weight loss |
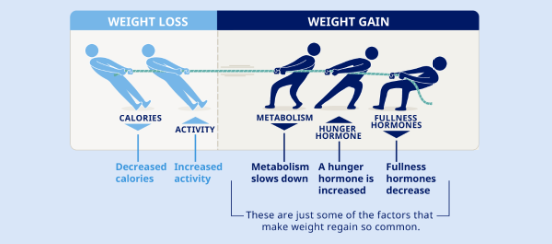
Weight management is like a tug-of-war because after weight loss, the body fights to put weight back on.3,4 Although people with obesity may achieve weight loss by reducing calories and increasing physical activity, metabolic and hormonal responses make weight loss difficult to maintain.3,4 Here’s how that works: 1. The metabolism slows down and gets more efficient, requiring fewer calories3 2. The body increases the hunger hormone ghrelin, which tries to induce calorie intake3,4 3. Fullness hormones that tell the brain it is time to stop eating are decreased3,4 |
| In fact, in people with obesity who have lost weight, the body will try to put weight back on for at least 12 months.4 |
| Multiple factors affect weight loss and weight maintenance |
In addition to the mechanisms described above, there are other factors that affect weight maintenance, such as: 1. Genetics, which may play an important role in the amount of weight gained5,6 2. Behavior, such as lack of sleep or physical activity7 3. Environment, which may make eating a healthy diet and exercising challenging6,7 |
As you can see, obesity is driven by many factors that contribute to its widespread prevalence and complexity.8,9
For additional information about the value of chronic weight management to your organization and to download resources you can use to help improve, maintain, and monitor health and wellness, please visit Novo Nordisk Works™.
For additional information about the value of chronic weight management to your organization, please contact us at laura.wicker@pbghpa.org or visit PBGH – Education, Advocacy, and Group Purchasing Solutions.
References: 1. Recognition of obesity as a disease. American Medical Association website. https://policysearch.ama-assn.org/policyfinder/detail/H-440.842?uri=%2FAMADoc%2FHOD.xml-0-3858.xml. Accessed December 7, 2020. 2. Mechanick JI, Garber AJ, Handelsman Y, Garvey WT. American Association of Clinical Endocrinologists’ position statement on obesity and obesity medicine. Endocr Pract. 2012;18(5):642-648. 3. Lam YY, Ravussin E. Analysis of energy metabolism in humans: a review of methodologies. Mol Metab. 2016;5(11):1057-1071. 4. Sumithran P, Prendergast LA, Delbridge E, et al. Long-term persistence of hormonal adaptations to weight loss. N Engl J Med. 2011;365(17):1597-1604. 5. Hebebrand J, Hinney A, Knoll N, Volckmar AL, Scherag A. Molecular genetic aspects of weight regulation. Dtsch Arztebl Int. 2013;110(19):338-344. 6. Bray GA, Kim KK, Wilding JPH. Obesity: a chronic relapsing progressive disease process. A position statement of the World Obesity Federation. Obes Rev. 2017;18(7):715-723. 7. Schwartz MW, Seeley RJ, Zeltser LM, et al. Obesity pathogenesis: an Endocrine Society Scientific Statement. Endocr Rev. 2017;38(4):267-296. 8. Jensen MD, Ryan DH, Apovian CM, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; The Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation. 2014;24(25 suppl 2):S102-S138. 9. Adult obesity prevalence maps. Centers for Disease Control and Prevention website. https://www.cdc.gov/obesity/data/prevalence-maps.html. Accessed December 7, 2020.
Post a Comment